Cardiology
Hepatojugular Reflux
‘A must do in the investigation of ascites’
Ascites is the abnormal accumulation of fluid in the peritoneal cavity. There are multiple causes for this condition and investigation of such cases is therefore complex.
Fluid can accumulate in the peritoneal cavity as a result of haemorrhage, infection/inflammation or progressive extravasation from the vascular space. The latter can be due to increased hydrostatic pressure, decreased oncotic pressure or increased vascular permeability.
One often forgotten or overlooked cause for the development of ascites is heart disease/failure. Any cardiac disease leading to elevated right sided pressures may compromise the process of systemic venous drainage increasing the pressure in the caudal vena cava. This process will ultimately result in extravasation of plasma over the pourable hepatic sinusoids leading to the accumulation of a modified transudate in the peritoneal cavity (ascites).
Advanced cardiac disease is suspected by detection of a murmur or an arrhythmia on physical examination (i.e. dilated cardiomyopathy, end stage mitral valve disease) but pericardial disease typically fails to produce these more common clinical indicators of heart disease. Pericardial effusion is in fact the most common cause of right sided heart failure by creating cardiac tamponade, a process that refers to the collapse of the right atrium under the increased intra pericardial pressures created by pericardial fluid that dramatically compromises venous return to the heart leading to ascites.
How to perform the hepatojugular reflux test?
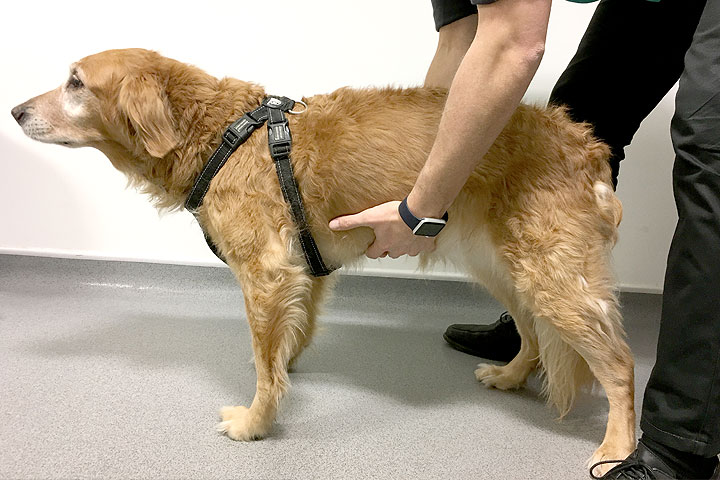
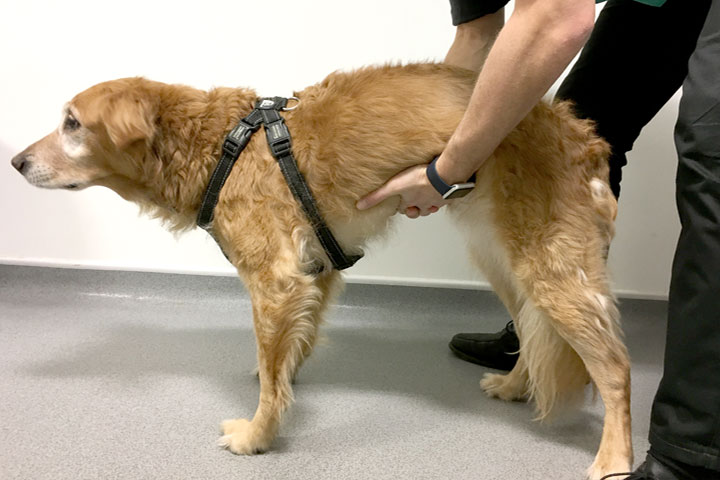
Clip the patient’s jugular area and identify the jugular vein by raising it a few times as in preparation for a phlebotomy. With the patient in a standing position put pressure on the caudal vena cava by lifting the patient’s abdomen whilst monitoring the jugular vein.
How to interpret the hepatojugular reflux test?
In a normal patient (normal right atrial pressure and no restriction dilation) the pressure created to the caudal vena cava will be accommodated by the right atrium and right atrial appendage with no pressure transmitted to the jugular vein (the jugular vein will not be raised). This means that the patient’s ascites is not caused by increased hydrostatic pressures resulting from heart disease/cardiac tamponade and further non-cardiac investigation should therefore be prioritised.
In a patient with markedly increased right atrial pressures, cardiac tamponade or any process compromising right atrial or right auricular appendage dilation (i.e. space occupying mass) the pressure applied to the caudal vena cava will be directly transmitted to the jugular veins causing it to dilate/raise. This means that the patient’s ascites is caused by heart disease (increased hydrostatic pressures) and cardiac investigation (echocardiography) should be prioritised.
Case Advice or Arranging a Referral
If you are a veterinary professional and would like to discuss a case with one of our team, or require pre-referral advice about a patient, please call 01883 741449. Alternatively, to refer a case, please use the online referral form