Soft Tissue Surgery
Vacuum Assisted Closure
Vacuum assisted closure (VAC) or negative pressure wound therapy (NPWT) is a simple but effective method to promote rapid wound healing. It has been shown to be effective for management of large, complex, acute wounds as well as chronic wounds that have failed to heal by conventional methods. It is also commonly used to stabilise free skin grafts following placement.
How does it work?
VAC is a treatment modality for management of wounds rather than a wound dressing, and works through application of negative pressure to the wound bed via open-cell polyurethane foam dressing (alternatively gauze can be used).
The foam acts as the wound contact material, filling the wound and allowing even distribution of the negative pressure over the wound bed. It is then connected via a suction tube to a canister, which fits on the side of the vacuum pump unit. The whole system is reliant on there being an effective seal around the dressing and this is achieved using the VAC semi-permeable film drape. Once the seal has been obtained, the pump can be set to deliver continuous or intermittent pressures, ranging from 50mmHg to 200mmHg.
Use of VAC results in decreased interstitial oedema and bacterial load, improved circulation and rapid formation of healthy granulation tissue. Among other mechanisms of action, subatmospheric pressure deforms tissue, which responds to mechanical tension by promoting angiogenesis and fibroplasia (proliferation of tissue and blood supply). This occurs in a closed and controlled environment with appropriate moisture and temperature, and free from further contamination.
The VAC system is usually removed, or the foam dressing is changed, 2-5 days following placement once healthy granulation tissue is present and before it adheres to the wound bed. Once healthy granulation tissue is present the wound can be closed surgically, have a graft placed, or allowed to heal by second intention.
Which wounds can benefit from VAC therapy?
Almost any type of wound can be treated with VAC, provided that a seal can be obtained and maintained during therapy. VAC is most commonly used on distal extremity shearing and degloving traumatic wounds, and to stabilise free skin grafts. It has also been used successfully to promote the formation of smooth granulation tissue in other traumatic wounds, burns, chronic non-healing wounds, abdominal and thoracic wounds, compartment syndrome and surgical dehiscence.
However, because VAC therapy promotes cell proliferation and applies suction to the wound bed, it is contraindicated in the presence of cancer, fistulas or exposed large blood vessels that can rupture. The presence of abundant necrotic or severely infected tissue is also a contraindication for the use of VAC and initial open wound management may be recommended. VAC should be used with care with patients suffering from bleeding disorders.
Conclusion
VAC therapy allows early appearance and improved quality of granulation tissue and may reduce overall cost though decreased frequency of dressing changes and reduced time to wound reconstruction and hospitalisation time.
CASE EXAMPLE
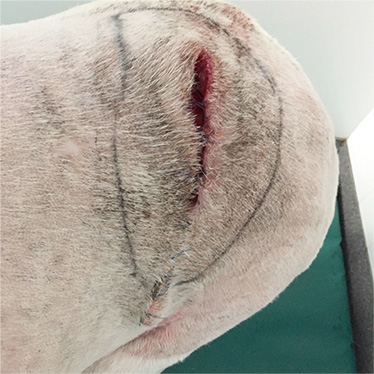
Oscar is an 8-year-old boxer that was presented for management of an open wound secondary to breakdown of a previous surgical site on the dorsal lumbar/left flank area. The wound is characterised by the presence of severe under-running and infection.
If you have any questions or would like advice on a case please call our dedicated vet line on 01883 741449 and ask to speak to one of our Soft Tissue Surgery team.
Note the presence of the wound and outlined area of under-running.
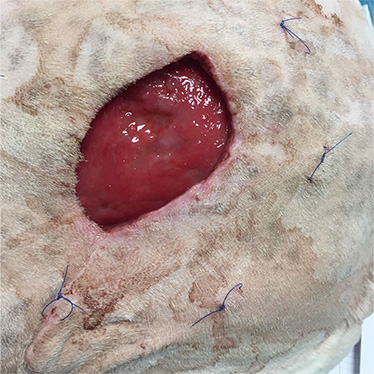
Note the unhealthy appearance of the granulation tissue. A bacterial culture grew an infection by Staphylococci and appropriate antibiotherapy was initiated.
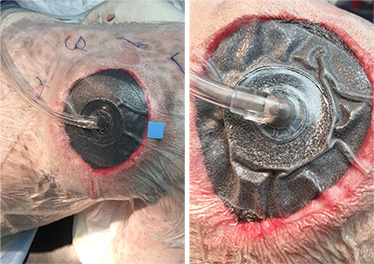
The wound was managed with VAC therapy. Note the appearance of the VAC during placement before and during negative pressure is created.
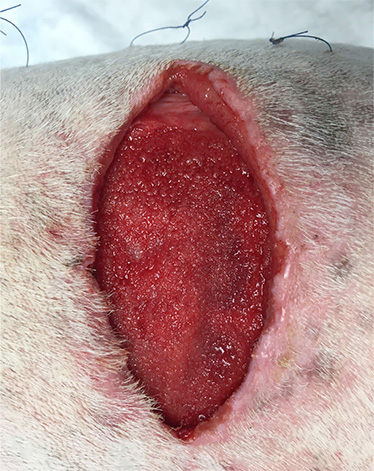
Note the appearance of the granulation tissue following VAC treatment. It is much more vascular and vibrant, and the dead space has virtually disappeared. The wound is ready for surgical closure.
Case Advice or Arranging a Referral
If you are a veterinary professional and would like to discuss a case with one of our team, or require pre-referral advice about a patient, please call 01883 741449. Alternatively, to refer a case, please use the online referral form