What is atopic dermatitis?
Allergic diseases result when the body’s immune system, which is usually responsible for defence against foreign organisms like viruses and bacteria, reacts to harmless substances that the majority of the population tolerate without problems. In the case of atopic dermatitis, an inappropriate immune response is produced to environmental substances and the resulting inflammation causes skin disease. The equivalent disease in humans is called atopic eczema, and this is a relatively common disease in the western world. Atopic dermatitis is one of the most common allergic skin diseases in dogs and cats.
Atopic dermatitis is hereditary, and there are certain breeds of dog such as West Highland White Terriers, Labradors, Chinese Shar Peis and Springer Spaniels that are more prone to develop the disease. Skin disease usually presents with itching, and very commonly affects the face, ears, feet, armpits and tummy. Recurrent ear infections are also very common, and some dogs with atopic dermatitis only have ear disease (figure 1). The inflammation within the skin causes redness, rashes, increased pigmentation (darkening of the skin) and recurrent infections. Skin disease usually develops between the ages of 6 months and 3 years.
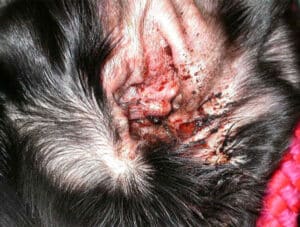
Figure 1: A severely inflamed ear due to infection and underlying allergy
In some affected animals, the allergic reaction can also cause eye problems such as conjunctivitis or respiratory signs such as sneezing. In all other respects, affected animals remain healthy, as atopic dermatitis does not affect other body organs.
What are the most common causes of atopic dermatitis?
The most common substances (allergens) triggering allergic reactions in northern European countries are the microscopic house dust and storage mites. These are tiny mites, invisible to the naked eye, that live in the home environment in places such as human clothes, furniture and carpets. These mites do not normally cause a problem, but animals with atopic dermatitis develop an allergic reaction to their presence. As these mites are present all year round, mite allergies usually result in skin disease that is all year round. Atopic dermatitis can also result from reactions to seasonal substances such as grass, weed or tree pollens. These reactions, which are rather like hay fever in humans, often result in skin disease that is at its worst during the spring/summer months.
How is it diagnosed?
Atopic dermatitis can be diagnosed following a thorough evaluation of the patient’s history, assessment of the patient’s clinical signs and elimination of a number of other similar diseases. Unfortunately, there is no single diagnostic test that definitively diagnoses the condition.
What are the treatments available?
Much like the human allergic diseases of hay fever, eczema and asthma, atopic dermatitis in animals cannot be cured. Patients with this disease have it for the duration of their lives and skin disease has to be managed in the long term. Skin disease can however be managed very effectively in the vast majority of patients.
Treatments for atopic dermatitis aim to reduce the over-active immune system and also improve the barrier of the skin to prevent further penetration of the causative substances (allergens). These treatments do not ‘cure’ the allergy, but aim to improve the patient’s clinical signs and comfort.
There are many different treatments and combinations of treatments for this, all with their own advantages and disadvantages, and their use can be discussed in detail with the dermatology Specialist.
Some dogs and cats with atopic dermatitis can also benefit from a treatment called immunotherapy, which is otherwise known as a desensitising vaccine. This is a long-term treatment option usually given by injection over a period of 9 months to 1 year, with the aim of reducing the over-active immune response. Injections are given under the skin and start off at intervals of 2 weeks before being spaced out to monthly injections. To have the information required to make up this treatment, allergy testing must be performed first. Allergy testing is usually in the form of an intradermal allergy test (figure 2), which is rather like skin prick-testing in people. However, it can alternatively be a blood test, used to detect circulating levels of antibodies. The intradermal test is performed under light sedation and involves injecting a panel of allergens into the skin to see if a reaction occurs. Both this and the blood test aim to identify possible triggering substances (allergens) which can then be used to formulate immunotherapy for the patient. Whilst immunotherapy is not effective in all animals, it can provide a drug-free way of controlling atopic dermatitis with very little risk of long term side effects.

Figure 2: An intradermal test on the clipped chest of a dog performed under light sedation
What is the outlook/prognosis?
In the vast majority of cases, atopic dermatitis can be controlled very well, and dogs can lead a normal and healthy life. As atopic dermatitis is a lifelong condition, periodic re-examinations with a dermatologist throughout the animal’s life are recommended to maintain close control over the disease and its clinical signs.
If you have any queries or concerns, please do not hesitate to contact us.
Arranging a referral for your pet
If you would like to refer your pet to see one of our Specialists please visit our Arranging a Referral page.