
What is the cornea?
The cornea is the clear window of the eye. It is a delicate structure which is less than a millimetre thick. In order to be transparent, the cornea has no blood vessels. It consists of three layers which are arranged like those of a sandwich. The three layers comprise:
- The epithelium – this is the thin outer ‘skin’ of the cornea
- The stroma which is the much thicker middle layer of the ‘sandwich’
- The endothelium – this is the inner layer of the cornea and is very thin indeed (only one cell thick)
What is a corneal ulcer?
Any injury involving the cornea can be described as an ulcer. Generally, corneal ulcers are described as superficial or deep, depending on whether they just involve the outer skin (the epithelium) – in which case they are called superficial ulcers, or whether they extend into the middle layer (the stroma) – in which case they are called deep ulcers.
Corneal ulceration is a painful condition which, if not treated correctly, can lead to blindness and even loss of the eye. The cornea normally has no blood vessels and as a result it is more easily infected than many other parts of the body. In addition, poor tear production (‘dry eye’) can make the cornea more liable to infection. In the presence of infection (and in some other circumstances), deepening of an ulcer may occur, sometimes very rapidly, and this may ultimately lead to rupture (bursting) of the eyeball. In this event the eye collapses due to leakage of fluid – the contents of the eyeball may prolapse through the perforation.
In cases where a deep ulcer is developing it is often necessary to perform surgery in order to prevent perforation and rupture of the eye. Such surgery will often involve the placement of a conjunctival pedicle graft into the corneal ulcer.
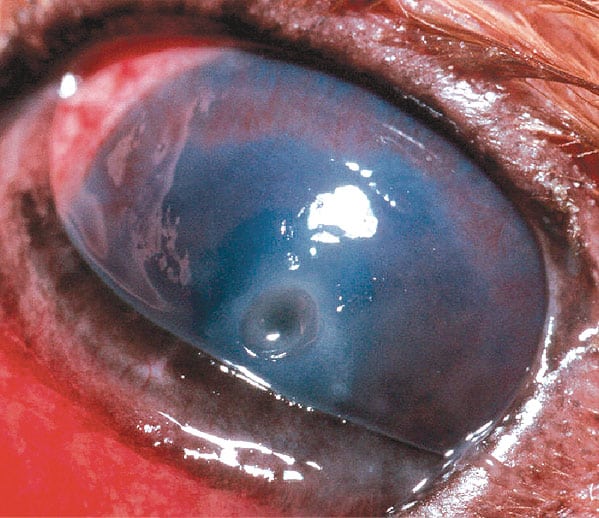
A deep corneal ulcer in a Cavalier King Charles Spaniel
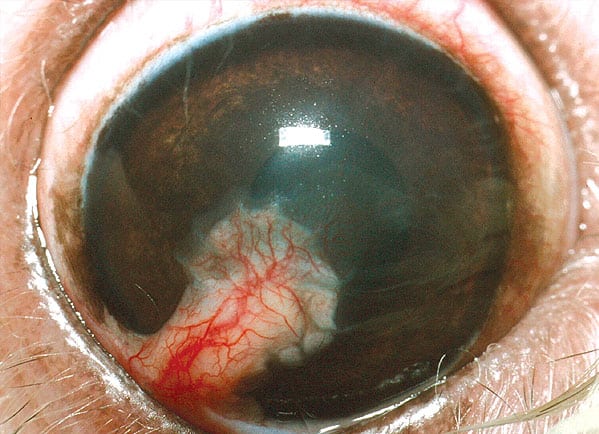
A conjunctival pedicle graft a few weeks after surgery
What is a conjunctival pedicle graft?
The conjunctiva is a thin membrane that covers the white of the eye. The conjunctiva has many blood vessels in it, although in the normal eye it is only lightly pink. However, it may become bright red due to irritation or inflammation of the eye.
In cases of rapidly progressive corneal ulcers, it is possible to surgically create a stalk or ‘pedicle’ of conjunctiva which can then be stitched into the corneal ulcer. The pedicle of conjunctiva not only provides some stability for the weakened cornea but also brings blood vessels (carrying healing cells and antibodies) right to the ulcer – this helps to fight infection.
What does the placement of a conjunctival pedicle graft involve?
In order to place a conjunctival pedicle graft, the patient has to be given a general anaesthetic. Once the patient is asleep, the area around the eye may be clipped. During the anaesthetic, the patient’s heart rate, blood pressure and blood oxygen concentration are monitored and a fluid infusion is given intravenously to maintain good blood circulation.
The operation is carried out under the operating microscope to allow visualisation and delicate handling of the eye. A flap of conjunctiva is cut free with fine scissors and rotated to fit into the corneal ulcer, which has first been surgically cleared of any unhealthy and infected tissue. The conjunctival flap is stitched into the wound with very fine suture material (as thin or thinner than a hair).
What aftercare will be required?
Post-operatively, the eye may be a little sore and swollen. The graft will be visible as a pink or reddish ‘blob’ on the cornea. A small amount of blood-tinged discharge may be produced from the eye, but this usually reduces after two or three days. The patient needs to wear an Elizabethan collar to prevent damage to the eye by rubbing or scratching.
Gentle cleaning around the eye with wet cotton wool twice daily is recommended. Antibiotic ointment or drops are generally applied to the eye for approximately ten days post-operatively. A short course of antibiotic tablets and mild painkillers may be dispensed.
Whilst the eyelid swelling will settle over the first week, it is possible that the graft will become more red as it grows into the surrounding cornea. This is generally temporary and the graft will then become pink again over time. It will take a few months for the eye to fully settle down and for the cornea to become as clear as possible.
Are there possible unwanted side-effects of a conjunctival pedicle graft?
As the graft carries blood vessels, it is likely to lead to an area of at least partial corneal scarring. In some patients brown pigment may grow onto the cornea from the graft. The degree of corneal scarring and the effect that this has on vision largely depends on the original size of the corneal ulcer. It may be possible to remove the pedicle or stalk that connects the grafted area with the conjunctiva under local anaesthesia. This may then reduce the degree of clouding in the cornea due to the graft. In some patients, a second procedure is recommended to remove as much of the graft as possible to clear the cornea. In most cases, the patient will retain enough clear cornea to have reasonable vision in the operated eye.
How successful is the operation?
The application of a conjunctival pedicle graft is usually a very successful operation, and failure to stop progression of the corneal ulcer is rare. In some cases with severe infection or large ulcers, however, the graft may fail and consequently detach from the cornea. A second operation can be carried out under these circumstances, and a new graft is put in its place. Complete failure of the operation with loss of the eye is very rare.
Could my own veterinary surgeon apply a conjunctival pedicle graft?
The application of a conjunctival pedicle graft to a corneal ulcer is a procedure that requires a skilled and experienced micro-surgeon, as well as equipment for magnification and illumination, and fine surgical instruments that will not damage the delicate eye tissues. For this reason most general practitioners will recommend referral to an ophthalmic specialist for this procedure.
Do I have to return to the eye specialist for the aftercare?
After an eye has developed a serious disease which has required a major operation, it is best to have its progress checked by the specialist. The number of re-visits will depend upon the severity of the problem, the post-operative progress and the underlying cause of the ulceration. In many cases only two or three re-visits will be required. In more complex cases there may be a need to continue with further check-ups from time to time. This will be discussed with you by the specialist at each stage of treatment.
If you have any queries or concerns, please do not hesitate to contact us.
Arranging a referral for your pet
If you would like to refer your pet to see one of our Specialists please visit our Arranging a Referral page.