
Canine malignant mammary tumours appear to be increasingly prevalent. This may reflect changes in neutering recommendations and/or the influx of dogs rescued from abroad, which are less likely to be neutered early in life. In this Focus on… piece, we hope to dispel some common misconceptions about mammary cancer and to give an overview of current best practice.
In our opinion, these are the issues that generate greatest controversy or that merit greatest attention:
- Link between neutering and mammary neoplasia
- Histological grade of canine mammary tumours
- What surgery should be performed
- Inflammatory mammary carcinoma
Neutering and mammary cancer
We do know that…
- The risk of mammary cancer is reduced in bitches which are neutered before the age of 2.5 years
- This risk is reduced further with earlier neutering with a presumed maximal cancer prevention benefit in bitches spayed before their first oestrus
However, the quantitative assessments of the degree of protection afforded by early neutering are extremely weak, being based upon very low case numbers. Furthermore, there are many good reasons not to neuter early.
Neutering at the time of surgery
We are often asked about whether to neuter a bitch at the time of mammary tumour removal.
We don’t have a one-size-fits-all answer for this. If the surgery is straightforward, there are benefits of spaying at the same time as tumour removal. If either the mammary tumour surgery or the ovariohysterectomy is expected to be complex or prolonged, avoid performing the two concurrently. If ovariohysterectomy is performed, it should always be done first without compromising the subsequent tumour removal. It is critical that the act of spaying does not allow seeding of the tumour into the peritoneum.
Histological grade
Canine mammary carcinoma grade has enormous prognostic significance. Over 50% of dogs with grade III tumours will die of their disease compared to 15% with grade II tumours and almost none with grade I tumours. If your report doesn’t mention the grade, ask for it!
- Dogs which have grade I tumours removed are generally cured of their cancer. However, they may develop new independent mammary masses. We suggest serial monitoring evaluations once every six months at least.
- Dogs with grade II tumours have a higher likelihood of distant metastasis and recurrence. Consideration should be given to chemotherapy or further surgery. Please contact us if you have a case like this and we would be happy to help.
- Dogs with grade III masses have a high risk of metastasis and recurrence and therefore would logically appear to benefit from chemotherapy. Multiple chemotherapy strategies have been described, but the benefit to this treatment remains unproven.
What kind of surgery should I be performing?
In dogs, almost all tumours under 1cm and most tumours under 3cm will be cured by surgery which achieves a 1cm margin around the mass. Excision also allows histopathological examination and diagnosis. The surgery that should be performed is then the simplest surgery which achieves this margin. For caudal glands, it might be less traumatic to remove glands 4 and 5 than it would be to transect the gland at the measured 1cm mark. In that case, mammectomy is preferred over nodulectomy.
However, if there are any of the following features, excision should not be the first step.
- Tumour diameter over 3cm
- Lymph node enlargement (always check the inguinal and axillary lymph nodes)
- Fixation of the mass
- Indistinct or irregular tumour boundaries
- Multiplicity of nodules
- Inflammatory features
Referral should be considered for these cases. We would recommend a biopsy of the mass to define the histological type and grade. We would recommend thoracic +/- abdominal imaging and FNA of the lymph nodes to ensure that surgery would be beneficial; decision-making concerning the precise imaging evaluations performed is driven by the results of biopsy. In the absence of evidence of metastasis, the surgical recommendations are broadly similar to those for less threatening masses but the margin of removal is increased. Body wall resection is important if the mass is fixed to deeper tissues. Surgical margins of 2-3cm are recommended with larger and more aggressive mammary tumours.

Complete unilateral or bilateral mammary excision is rarely performed in dogs (contrast cats). The procedure is associated with high morbidity and limited benefit.
Inflammatory mammary carcinoma
Mammary cancer comprises a spectrum of neoplastic diseases, but one clinical entity which deserves particular attention is the inflammatory mammary carcinoma. This is an extremely aggressive and clinically distinct form of mammary cancer. Typically, the disease will start with some mild bloody discharge, pain and swelling. It is unusual to find an overt mass and it can be mistaken for mastitis. Inflammatory mammary carcinoma should be considered in any middle aged or older dog with these signs, especially if there no response to initial treatment. As the disease progresses, the skin ulcerates and often progresses into the groin as in the picture below. If you encounter this pattern of progression, please heed the alarm bells.
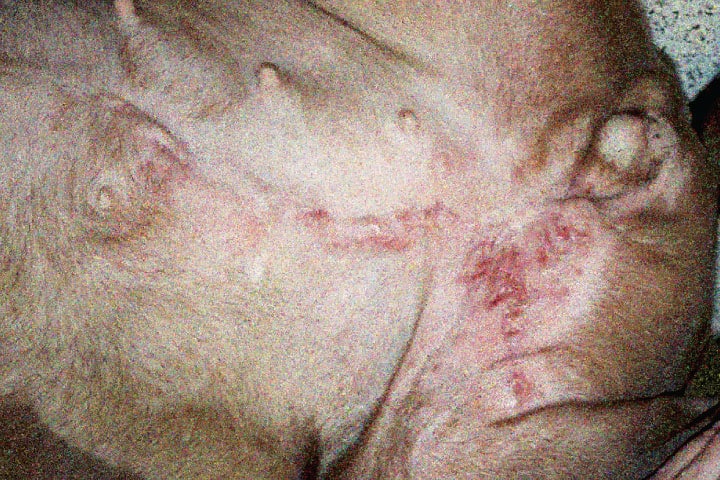
The picture also highlights the extremely rapid recurrence after surgery. This dog had a red, ulcerated mass removed from the caudal 4th and 5th glands only three weeks earlier. Surgery was not clinically useful in this dog. If you suspect inflammatory mammary carcinoma, we recommend a skin punch biopsy; cytology can be unreliable in this condition. Unfortunately, there are no successful treatment options for this cancer. Surgery is not useful and neither is conventional chemotherapy. Inflammatory carcinomas have highly upregulated COX enzymes; COX inhibitor therapy is currently the most effective treatment we have. NSAIDs palliate the pain associated with these tumours and can delay tumour progression. Additional analgesia will often be required; consider tramadol, paracetamol and/or amantadine. Radiotherapy may also be used, purely for analgesia and anecdotally, this can be effective.
Key messages
- Early neutering reduces the risk of mammary cancer. This should be balanced against other considerations
- There is a limited benefit to neutering at the same time as mammary tumour removal
- We have a clinical trial available for dogs with high-grade mammary carcinomas
- Mammary strips are generally not recommended
- Be mindful of the presenting signs associated with inflammatory mammary carcinomas
Case Advice or Arranging a Referral
If you are a veterinary professional and would like to discuss a case with one of our team, or require pre-referral advice about a patient, please call 01883 741449. Alternatively, to refer a case, please use the online referral form
About The Discipline
Oncology
Need case advice or have any questions?
If you have any questions or would like advice on a case please call our dedicated vet line on 01883 741449 and ask to speak to one of our Oncology team.
Advice is freely available, even if the case cannot be referred.
Oncology Team
Our Oncology Team offer a caring, multi-disciplinary approach to all medical and surgical conditions.