
Primary bone tumours in dogs are seen with alarming frequency, particularly in large and giant breeds. Tragically, many of those patients do not receive anti-cancer therapy.
This is a field with plenty of scope for improvement. Here we consider the elements of care for these patients in which greatest improvements can be made.
Diagram showing the classic history for a dog with a bone tumour prior to diagnosis
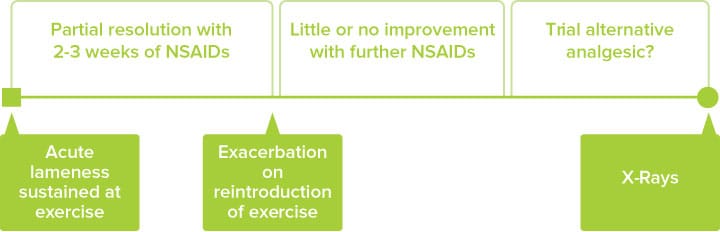
that unsuspecting owners of large or giant breed dogs will lay for you.
Ultimately, osteosarcoma is a nasty condition and if we are going to achieve better outcomes for patients we need to make some improvements in management. These are improvements that can be made by everyone; specialist and first-opinion practice must work together.
In our opinion these are the areas in which those improvements can be made:
1 Prevention
2 Early diagnosis
3 Correct diagnosis
4 Support for owners
5 Immunotherapy
1 Prevention
Did you know that neutering before growth plate closure increases the risk of osteosarcoma? Studies report up to a 3.8 times greater risk of tumour development in dogs neutered before the age of one year! This increased risk is greater in males and greatest in breeds already known to be at-risk, for example, Great Danes and Rottweilers. Cancer prevention is the best kind of cancer treatment. We believe that the risk of bone cancer should feature in any discussion of neutering in large and giant breed dogs.
2 Early diagnosis
The timeline depicted deliberately doesn’t feature actual time intervals. But you can imagine how long it would usually take to progress from initial ‘injury’ to first radiographic signs of osteosarcoma. In our experience from seeing many case histories, it’s usually about eight weeks. There are certain features of the clinical examination of a lame patient which should prompt early radiography, leading to a more rapid diagnosis.
Top Tip
Detailed examination of the affected limb should allow localisation of pain to the affected part of a limb. Osteosarcoma classically affects metaphyseal bone. This will manifest as pain in or near a joint. The severity of the pain often impedes further localisation. Using the contralateral limb as a comparator, check for bony asymmetry spanning a joint or localised to one bone in the joint.
Bony asymmetry:
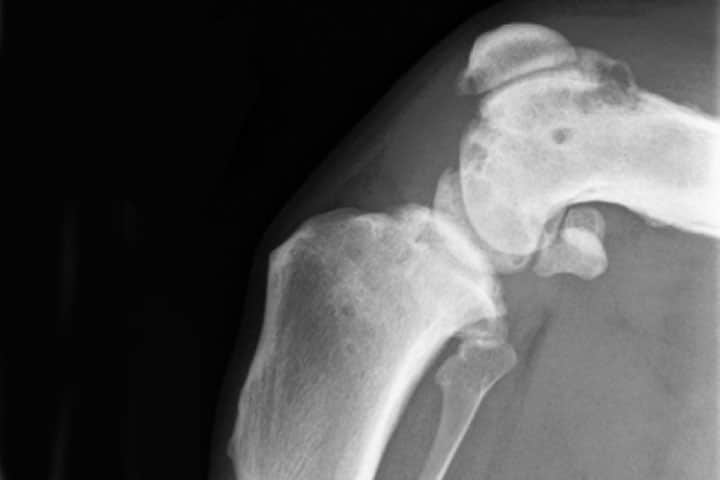
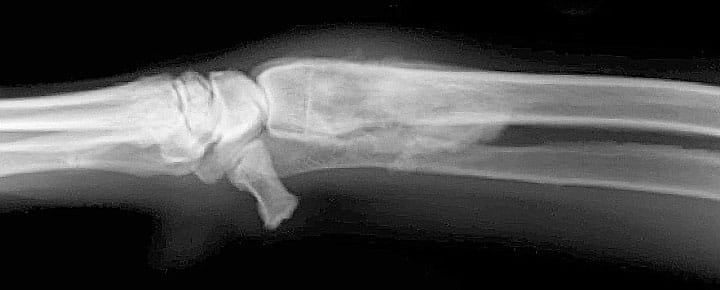
The presence of a painful bony swelling, especially if monostotic, should prompt radiography. Early diagnosis means appropriate analgesia is administered earlier. It may mean that surgical intervention is applied sooner and pain is completely removed. Common sense and every oncological principle tell us that it will also improve the likelihood of a favourable and lasting response to treatment.
3 Correct diagnosis
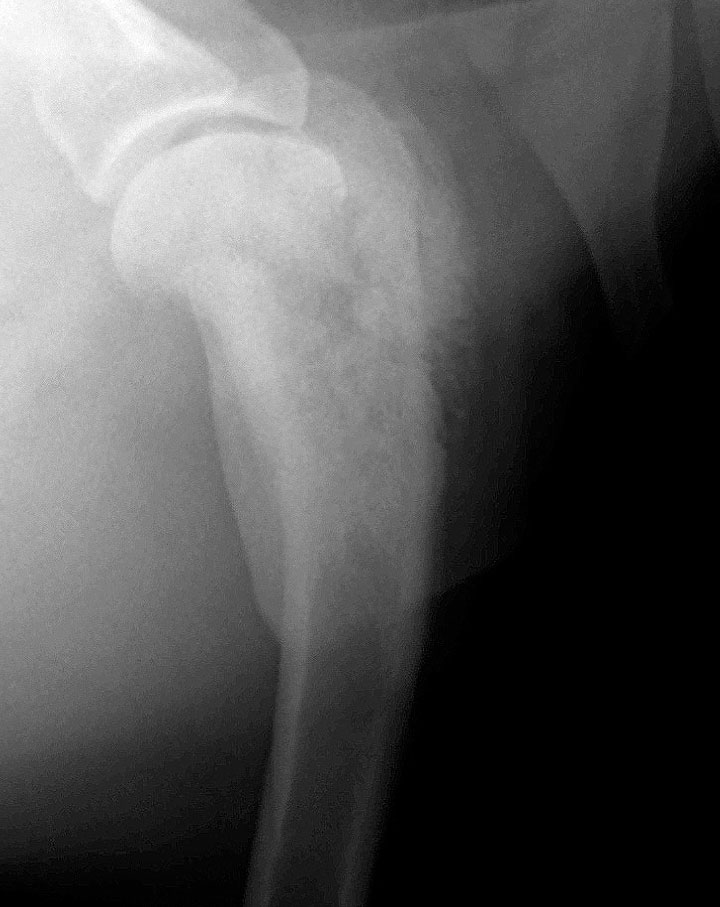
There was a time when we would say that any lytic bone lesion in the metaphyseal region of a long bone in a dog was osteosarcoma until proven otherwise. However, the prevalence of other primary bone tumours is changing and troublingly so. We see fewer osteosarcoma cases than ever before but more haemangiosarcoma, histiocytic sarcoma, chondrosarcoma and plasma cell tumour cases, all capable of manifesting in the classical osteosarcoma fashion. We strongly suspect that this is partly due to improvements in histological diagnosis. But it is of major importance. Clinical stage evaluations differ. Treatments and prognoses differ, potentially enormously.
Differential diagnosis:
- Osteosarcoma
- Histiocytic Sarcoma
- Chondrosarcoma
- Haemangiosarcoma
- Plasma Cell Tumour
- Lymphoma
- Myeloma
- Osteomyelitis
- Fungal Granuloma
- Metastasis (typically carcinoma)
There a number of options for achieving the diagnosis. Which is the correct one is case dependent. A fine needle aspirate is often diagnostic, can be less painful and quicker to perform, with more rapid results. It can be technically difficult though. A bone biopsy with a Jamshidi needle is the classic method. We would be happy to speak to you with advice on how to achieve a diagnosis at any time.
4 Support for owners
Limb amputation is a big deal for owners. For all of our confidence that stems from seeing these patients perform so well after surgery, owners will consistently fear that their pets will not enjoy a good quality of life following amputation. A recent study showed that 86% of owners who elected for amputation in their pets would make the same decision again and we find this figure will often give some reassurance.
Not all owners will choose amputation. It is vital, in our role as advocates for our patients, that accurate and clear advice is given concerning the alternatives.
In considering the options for a patient with a primary bone tumour, significant attention must be paid to the lifestyle and quality- of-life implications of treatment. There are a number of options for additional analgesia, such as bisphosphonate drugs, limb salvage and radiotherapy.
While much support and advice can be provided by specialists and experienced practitioners, another excellent source of support can be found among owners of patients with experience of the same diagnosis and the same management dilemmas.
5 Immunotherapy and future directions
With advances in diagnostic testing and treatment in other fields, we would expect an improvement in outcomes for canine osteosarcoma over time. The truth is that the outcomes for dogs with this condition and the standard of care have been static for the past 29 years. With chemotherapy post-amputation, the median survival is around 10-12 months, with 20% of dogs living for longer than 2 years.
This lack of improvement is not for want of trying. A number of novel therapies have been trialled, which were either unsuccessful (metronomic chemotherapy, Palladia) or are no longer available. Limb spare procedures are an advancement which can help dogs for which amputation is possible. However, high complication rates (up to 96%) and significant expense mean that these are often not the best choice.
At NDSR, we are currently enrolling for a trial using immunotherapy prior to amputation to try to direct the dog’s own immune system to the cancer cells in order to control its progression. This is combined with the normal standard of care (carboplatin). Early assessments appear very positive. Safety of the agent is proven and to date, there appears to be no risk of toxicity in recruited patients. We would of course be more than happy to discuss this with you.
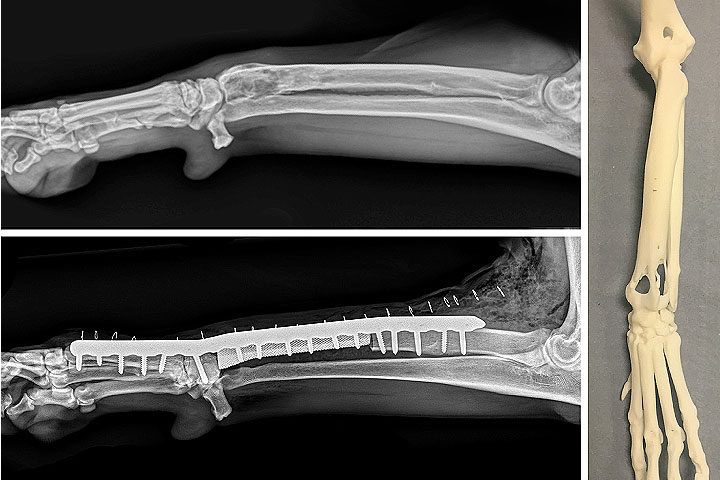
With the advent of 3D-printing technology, we are now able to offer customised endoprosthetic titanium implants for our osteosarcoma limb-salvage patients.
At present, we limit this to patients with distal radial osteosarcoma but this is a fast-moving field.
Key messages
- There is a significant increase in the risk of osteosarcoma in large and giant breed dogs neutered before achieving skeletal maturity
- Osteosarcoma should be considered in the mature patient whose lameness fails to respond as expected to rest and anti-inflammatory therapy
- Osteosarcoma classically affects the metaphyses of the long bones. It does not span the joint!
- Currently there is a clinical trial available for patients with suspected osteosarcoma. Telephone us to discuss: early assessments appear very positive
Case Advice or Arranging a Referral
If you are a veterinary professional and would like to discuss a case with one of our team, or require pre-referral advice about a patient, please call 01883 741449. Alternatively, to refer a case, please use the online referral form
About The Discipline
Oncology
Need case advice or have any questions?
If you have any questions or would like advice on a case please call our dedicated vet line on 01883 741449 and ask to speak to one of our Oncology team.
Advice is freely available, even if the case cannot be referred.
Oncology Team
Our Oncology Team offer a caring, multi-disciplinary approach to all medical and surgical conditions.